- Home
- News
- Features
- Topics
- Labor
- Management
- Opinions/Blogs
- Tools & Resources
Cost of Employer-Provided Health Insurance Up 9%
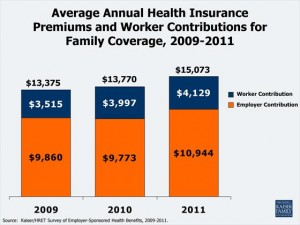
Annual premiums for employer-sponsored family health care insurance coverage increased 9% from 2010 to $15,073 this year, according to the Kaiser Family Foundation/Health Research & Educational Trust 2011 Employer Health Benefits Survey released Tuesday, 27 Sept. 2011.

On average, workers pay $4,129 and employers pay $10,944 toward those annual premiums.
Premiums increased significantly faster than workers’ wages (2.1%) and inflation (3.2%). Since 2001, family premiums have increased 113%, compared with 34% for workers’ wages and 27% for inflation.
“This year’s 9% increase in premiums is especially painful for workers and employers struggling through a weak recovery,” said Drew Altman, Kaiser president and CEO.
According to Maulik Joshi, president of HRET and senior VP for research at the American Hospital Association, “survey findings related to the impact of early provisions in health reform provide valuable insight for employers, providers, consumers, and policymakers as they prepare for additional provisions to take effect by 2014.”
The 13th annual Kaiser/HRET survey of small and large employers provides a detailed picture of trends in private health insurance costs and coverage. This year’s survey also looked at employers’ experiences with several already implemented provisions of the 2010 health reform law affecting employer coverage.
In particular, the survey estimates that employers added 2.3 million young adults to their parents’ family health insurance policies as a result of the health reform provision that allows young adults up to age 26 without employer coverage on their own to be covered as dependents on their parents’ plan. Young adults historically are more likely to be uninsured than any other age group.
“The law is helping millions of young adults to obtain health coverage,” said Gary Claxton, a Kaiser VP ive director of the Kaiser Initiative on Health Reform and Private Insurance. “In the past, many of these young adults would have lost coverage when they left home or graduated college.”
The study also found 31% of covered workers are in high-deductible health plans, facing deductibles for single coverage of at least $1,000, including 12% facing deductibles of at least $2,000. Covered workers in smaller firms, those with 3-199 workers. are more likely to face such high deductibles. Half of workers in smaller firms facing deductibles of at least $1,000, including 28% with deductibles of $2,000 or more.
These numbers in part reflect the rise of consumer-driven health care plans, which are high-deductible plans that include a tax-preferred savings options such as a Health Savings Account or Health Reimbursement Arrangement.
During the past two years, more companies have offered these plans, and the share of covered workers enrolled in this type of plan has doubled, from 8% in 2009 to 17% in 2011. Health care plans that can be used with a Health Savings Account have lower premiums than other plan types, but must have annual deductibles of at least $1,200 for an individual and $2,400 for a family this year.
Findings Related to Health Reform
The survey finds that 56% of covered workers are in “grandfathered” plans as defined under health care reform. Grandfathered plans are exempted from some health care reform requirements, including covering preventive benefits with no cost sharing and having an external appeals process. To obtain this status, employers cannot make significant changes to their plans that reduce benefits or increase employee cost.
One in four covered workers, 23%, are in plans that changed their cost-sharing requirements for preventive services as a result of a requirement of the health care reform law that non-grandfathered plans provide certain preventive benefits without cost sharing. In addition, 31% of covered workers are in plans that changed the list of preventive services due to health reform.
Other findings from the study include:
Worker-only coverage
Offer rate
Cost-sharing for office visits and drugs. Covered workers facing copayments for in-network physician office visits on average pay $22 for primary care and $32 for specialty care. For covered workers with three- and four-tier drug plans, average copayments are $10 for generic drugs, $29 for preferred brand-name drugs, $49 for non-preferred brand-name drugs, and $91 for specialty drugs.
Retiree health benefits. Among large companies, those with 200 or more workers, about one in four, 26%, offer retiree health benefits in 2011, unchanged from last year and down significantly from 32% in 2007.
Full survey results are available online at
- http://ehbs.kff.org
.
List your business in the premium web directory for free This website is listed under Human Resources Directory




